Setting the Stage for Flu’s Disappearing Act
Important points about U.S. flu surveillance, with examples from the 2009 H1N1 "pandemic"
In my first post on the disappearance of flu, I asserted:
Influenza was largely absent from surveillance reporting and detection for over a year due to Human Interference (HI), not Viral Interference (VI) or non-pharmaceutical interventions (NPIs)
Health agencies took actions and issued orders and guidance that account for the sudden drop and subsequent dissipation of flu tests being given and returning positive.
These steps were taken in the context of global and national influenza surveillance that is already coordinated and involves much uniformity.
In this post, I’ll “set the stage” for the disappearance by showing that U.S. flu surveillance data are not wholly objective or unbiased measures of disease prevalence or severity. Long-term patterns and the events of the 2009 swine flu/H1N1 pandemic1 help illustrate some of the ways human behaviors and decisions impact the data that are collected and reported.
The next post will focus on whether the 2019-2020 flu season was shaping up to be remarkable before covid-19 officially came on the scene.
Flu: The Longtime Star of the Surveillance Show
Influenza virus (a.k.a. “flu”) is one of the pathogens that the U.S. surveils or “keeps track of”. Before Covid-19 entered the theater, flu was the star of the show – and the focus of pandemic preparedness efforts.2 Flu surveillance is coordinated by the CDC, which produces reports using data from health departments in all 50 states.
The official “flu season” starts in October and ends in May.3 This is the period in which active surveillance occurs and weekly reports are issued. The variables are considered measures of whichever strains (known and unknown) are circulating — and the season’s overall severity. Three data points are prioritized in surveillance: ILI, testing, and flu/pneumonia deaths.
Influenza-Like Illness: Did You Stay or Did You Go?
Influenza-Like Illness (ILI) is a non-specific, clinical or empirical term defined as fever of 100 degrees and cough or sore throat. It isn’t test-dependent – that is, it has nothing to do with whether a person was given a flu test or tested positive for influenza. The definition casts a fairly wide net, with symptoms that could be caused by any number of things, including other respiratory agents.
The general pattern in the U.S. is for ILI to rise in the fall, peak in the winter, and decline in the spring. ILI data come from healthcare providers in outpatient settings who sign up to be sentinels.4 Each week, these sentinels report their total number of patient visits and total number of visits for ILI by age group. These numbers are represented as a proportion. For example, if 12,000 of 800,000 visits reported nationally for a week were for ILI, the ILI rate is 1.5%.5
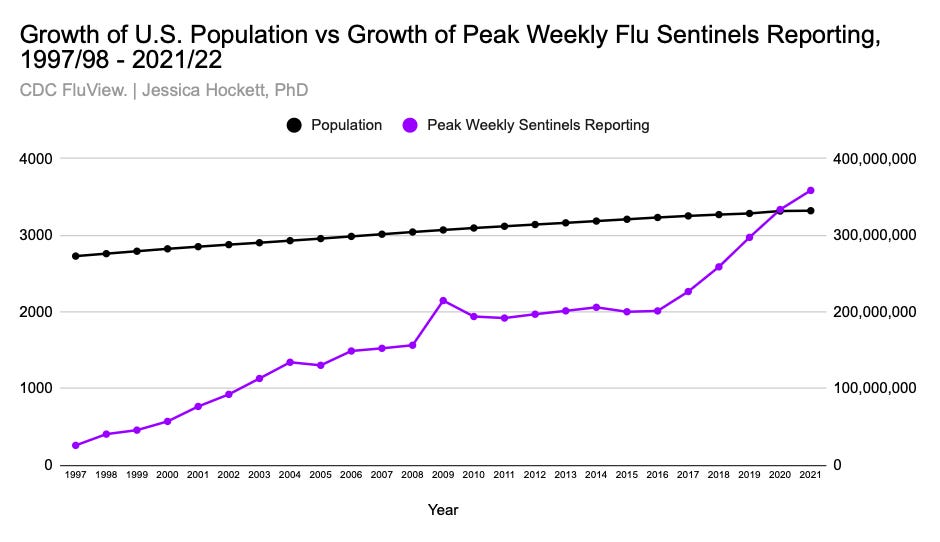
The number of sentinel providers in the U.S. has increased considerably since 1997, from less than 200 to over 3,500 (Figure 1). The H1N1 push in 2009 saw the biggest jump. Increases from 2017 onward are sharper than year-to-year increases before and after 2009-2010.
Figure 1
Whether and how “more” sentinels improves ILI as a surveillance tool - or saves lives and reduces disease burden - is unclear. (The evidence from influenza-attributed mortality, however, shows no evidence of decline in the past dozen years. If anything, there is an increase, which I discuss later in this post.)
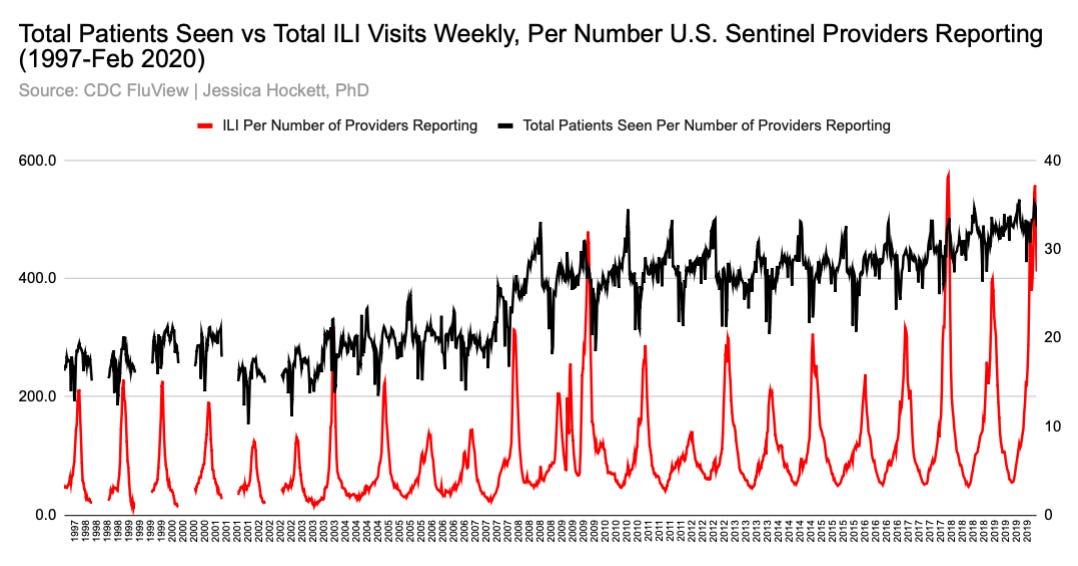
It’s possible the CDC’s ideal is a certain percentage of all outpatient healthcare providers. The number of outpatient facilities in the U.S. has grown over the years, as has the number of people seeking healthcare at such facilities, which could be why total visits and ILI visits per sentinel have increased (Figure 2).
Figure 2
Although ILI reflects how many people feel sick - and how sick those people are feeling - other factors shape whether someone seeks medical attention for flu-like illness. For example, having medical insurance or living close to a doctor’s office6 From a practical standpoint, we can imagine that social forces also play a role. Co-workers are saying “the flu is going around.” News media are panicking about hospitals being overrun with flu patients. Tweets and Facebook are swirling with talk of fatigue, sudden fever, and a cough that just won’t go away. All of these things can nudge people to seek (or avoid) healthcare for respiratory illness.
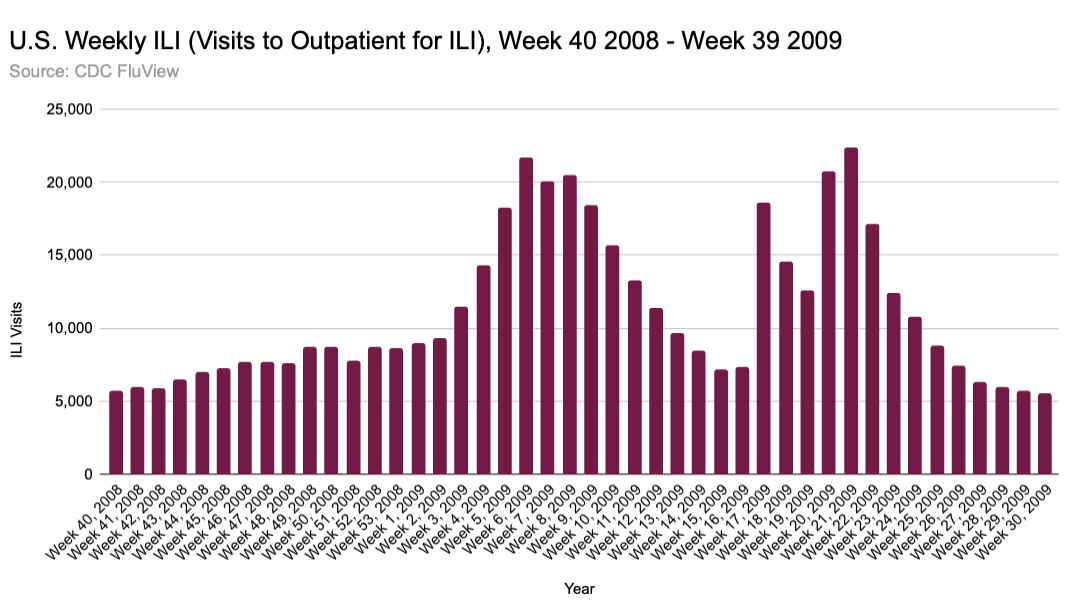
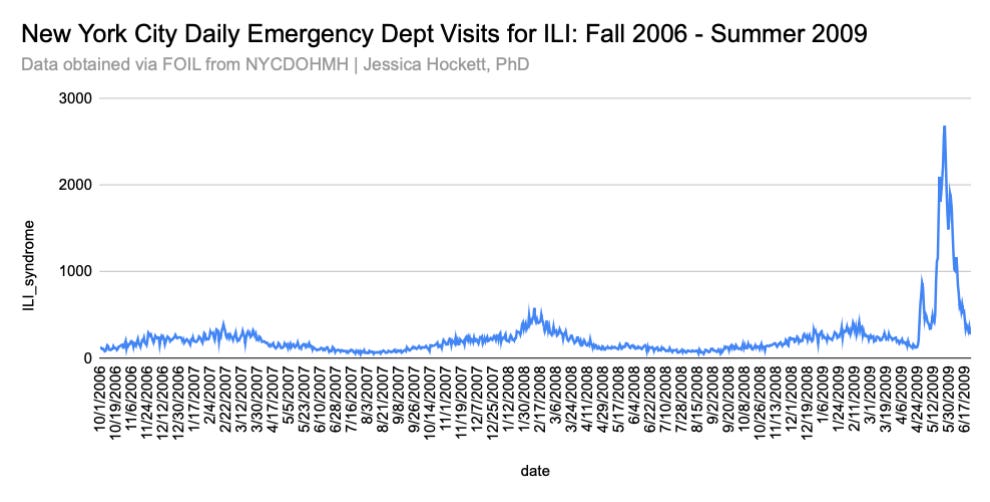
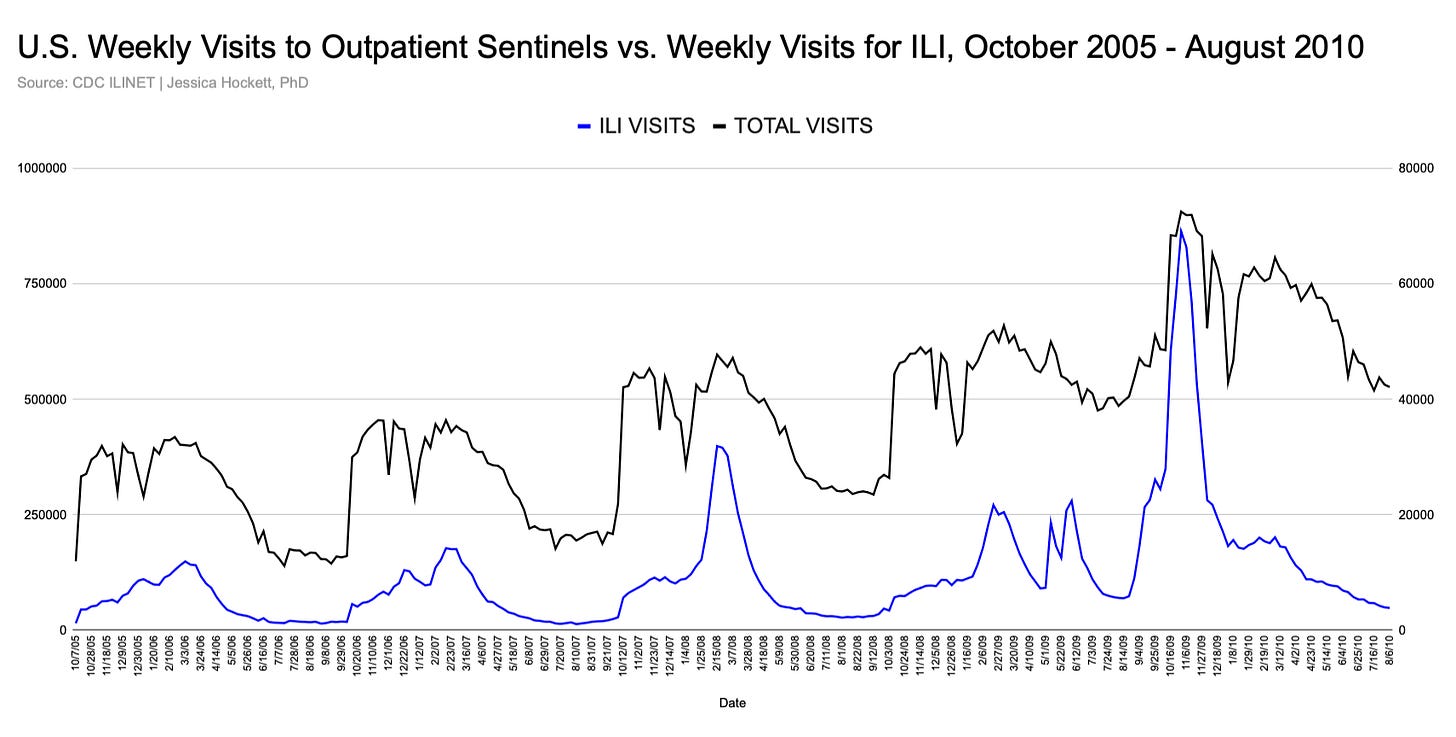
Announcements from government entities seem to have a big impact on ILI too. The 2008-09 season was nearly over when the WHO issued an emergency statement about swine flu. ILI visits shot up almost immediately (Figure 3). Daily emergency department ILI visits in New York City at the time show an even more dramatic spike (Figure 4).7
Figure 3
Figure 4
Especially without context, these data give the impression that swine flu (a.k.a. H1N1) dropped like a bomb. But viruses aren’t bombs, and the ILI data in these weeks are better characterized as non-viral stimuli triggering a change in people’s perception and behavior than sudden spread of a freshly-emerged pathogen. There were simultaneous jumps not only in different regions of the U.S., but in the U.K. and elsewhere. A purported H1N1 outbreak on a college campus in Delaware likewise shows ILI visits going up after students heard there was something to fear.
If the explanation for these conspicuous violations of seasonal patterns were biological, there should at least be a gradual increase in ILI leading up to the WHO statement. In early May, the agency changed its definition of an influenza pandemic from “an influenza pandemic occurs when a new influenza virus appears against which the human population has no immunity, resulting in several simultaneous epidemics worldwide with enormous numbers of deaths and illness” to “an influenza pandemic may occur when a new influenza virus appears against which the human population has no immunity.” This was apparently done after a CNN reporter asked about how a pandemic could be imminent without “enormous numbers of deaths and illness.” (Peter Doshi provides a good summary of what occurred.)
ILI’s susceptibility to external influences doesn’t render it a worthless measure. Rather, it means the data should never be divorced from contemporaneous events that occur or messages people receive. In the case of H1N1, people heard there was an off-season flu emergency and reacted by seeking healthcare for whatever mundane symptom(s) they might have otherwise ignored.
Flu Testing & Virologic Surveillance: To Test or Not to Test?
Flu testing is another variable reported via weekly surveillance. This includes the number of specimens tested for influenza, the number of specimens testing positive, the ratio between the two (percent positive), and the number of positive tests by type and subtypes.
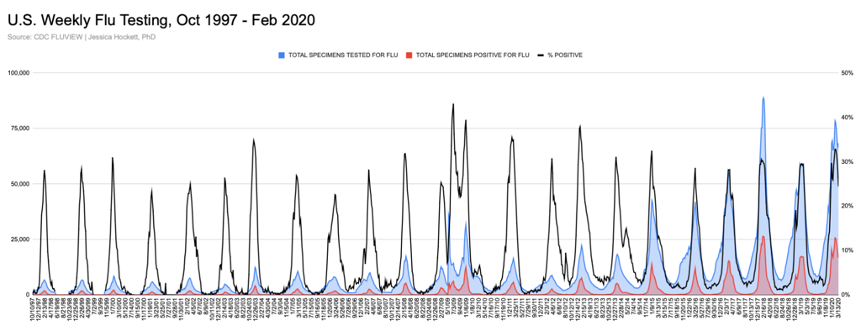
U.S. flu testing efforts increased considerably in two decades. Roughly 5,000 to 6,000 specimens tested by clinical and public health labs during peak season in 1997-1998 grew to nearly 90,000 tests in 2017-2018 (Figure 5). More testing has yielded a higher number of positive tests, with peak percent positivity between 30-40%8 (2009 is an exception I’ll explain in a bit.)
Figure 5
Like ILI, there is a degree of human judgment in and multiple outside forces acting on flu testing. Prior to the Covid Testing Complex, the decision to test a patient for flu seemed to be in the hands of the doctor who was seeing the patient. Signing up to be a flu sentinel provider came with a request to send a minimum number of specimens each week to a public lab for viral testing, but doctors didn’t typically test simply for the sake of testing. Testing in the absence of symptoms, testing everyone in the hospitals and weekly testing as a condition of employment – all things we’ve seen in the Covid Era - wasn’t the norm. Such “screening testing” dramatically elevates the number of false positives in the number of positives; the relationship has not been fully explained or characterized.
As one might expect under a coordinated surveillance program, when and who to test for flu is “directed.” Martin Neil and colleagues observed that CDC flu testing guidance pushes physicians toward or away from testing under certain circumstances and with some patient populations.9 Physicians are given different algorithms depending on whether flu is “circulating” or there is an “outbreak,” whether the patient is at high risk for flu complications, has certain conditions, and/or the results are necessary for treatment. This is not to say that physicians are simply following a formula; to be sure, each doctor exercises professional judgment and assesses individual patients or situations, but clearly there is a kind of conditioning steered by smaller groups of professionals.
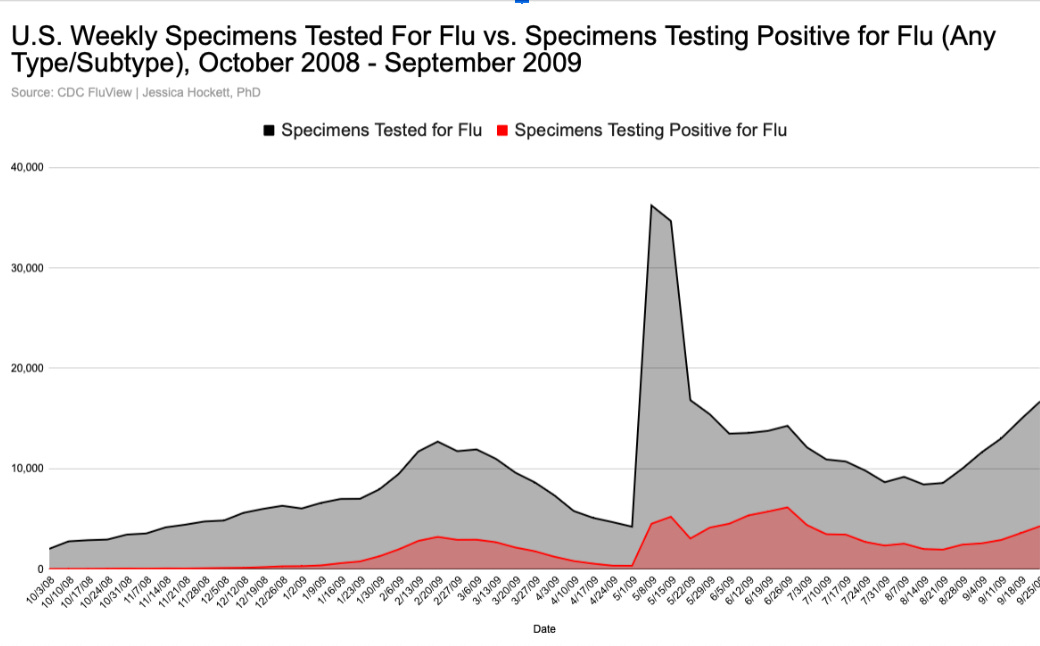
Public health alerts and orders arguably have an even bigger impact on flu testing than such guidance. This is especially true when an outbreak or emergency is declared. Shortly after the WHO issued its urgent announcement about the “pandemic swine flu,” the FDA authorized the first H1N1 test for emergency use. Apparently, the tests were ready to go, because the number of flu specimens tested immediately went vertical, tripling their seasonal peak in one week.10 Similar to ILI, there was no gradual increase of flu specimens tested that might suggest people were sick with an “emerging” flu strain (Figure 6).
Figure 6
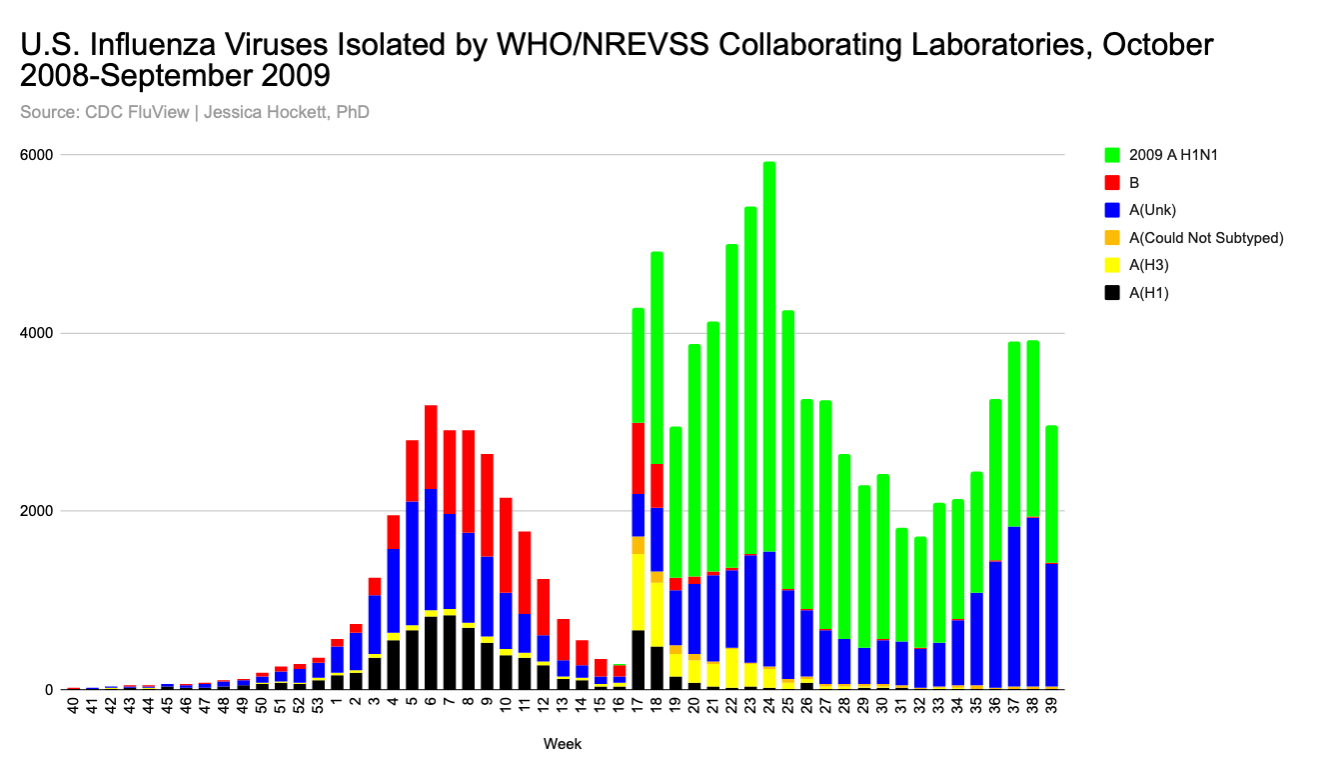
Virologic surveillance data for this period are comical.11 How does a version of flu fail to show up in ILI or the number of specimens tested, and then light up on the radar after people are told it’s on the scene? There is no plausible biological explanation for the explosion in positivity; it was driven by the test availability and testing. This is a big reason why, along with detection of the “novel” H1N1, we see increases in positivity of many other viruses in the flu stew (Figure 7).
Figure 7
As far as I know, prior to this advent of H1N1, a summer respiratory illness outbreak of this magnitude hadn’t been observed. An explanation for a flu bug skyrocketing at this time of year that I often hear is, “Because it was novel.” The more obvious explanation is, “By creating a test and testing a lot of specimens for something that was there all along.”12
Some people say 2009 H1N1 as an example of viral interference, with H1N1 snuffing out or pushing aside other strains. I see interference, but of an economic and political nature. The development of an H1N1 shot, which was initiated before the WHO alert and a test was approved.13 The shot debuted fairly quickly, in October, amidst controversy about the purported utility of mass testing, no less. In a scathing critique published in Forbes at the time, journalist Michael Fumento said the swine flu pandemic was partly a “CYA for the WHO.”
[The WHO] was losing credibility over the refusal of avian flu H5N1 to go pandemic and kill as many as 150 million people worldwide, as its "flu czar" had predicted in 2005. Around the world, nations stockpiled antiviral medicines and H5N1 vaccine.
So when pig flu conveniently appeared, the WHO essentially crossed out "avian," inserted "swine," and WHO Director-General Margaret Chan could boast: "The world can now reap the benefits of investments over the last five years in pandemic preparedness." October 9, 2009
In other words, there was a public health solution in need of a public health problem—and a need to show the solution worked.
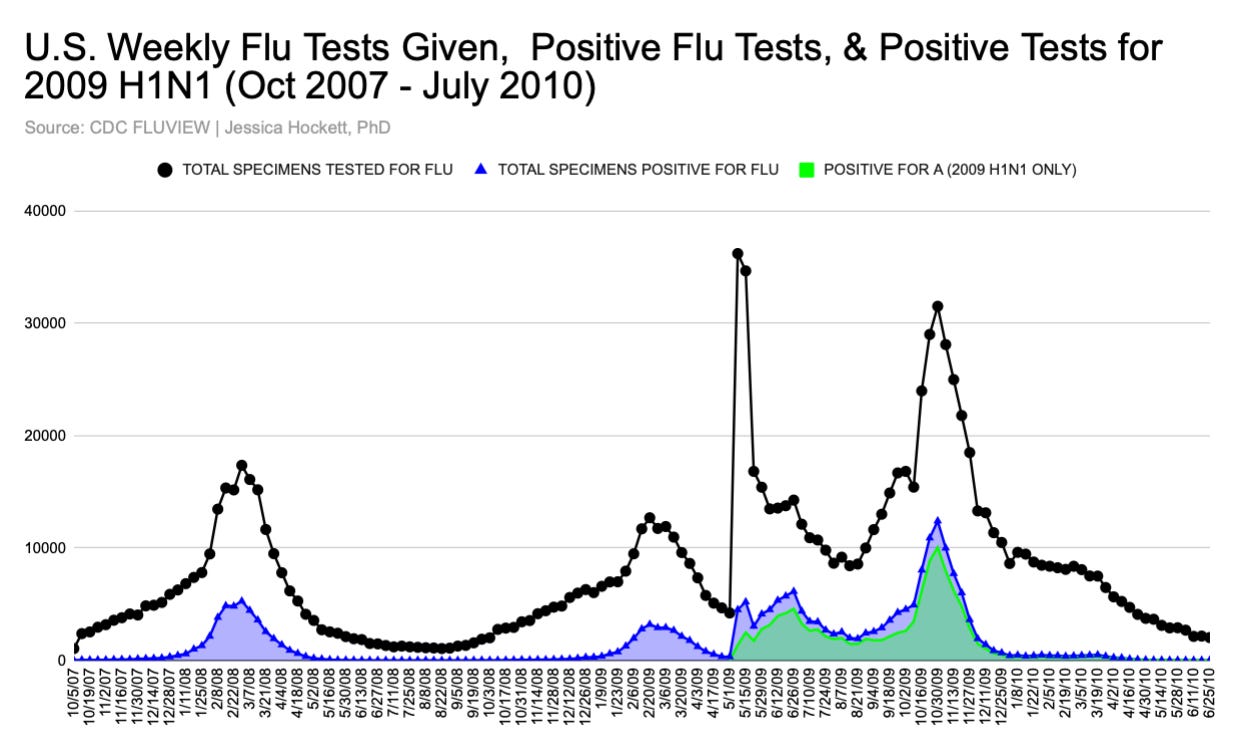
Looking back at the data, we see specimens tested for flu declined in December, as did positives and H1N1 positives (Figures 8 and 9). The timing is curious, since ILI and flu testing climbs and peaks in winter.
Figure 8
Figure 9
Outpatient visits were also highest in October, as were ILI visits, with public health authorities and media fomenting fear about a “second wave”. Total visits for any reason remained high in the winter months (i.e., there was no shortage of people coming in). Yet, ILI was lower than in past seasons, which makes no sense, because people were still dying of pneumonia in the hospital.
The CDC implicitly credited vaccination for the drop. Given ILI’s broad definition - and the motivation to show a new treatment was effective - there are reasons to believe that other factors were at play for the reduction in outpatient visits coded for flu-like illness.
All of this to say, the flu testing program has never been a pure or unbiased measure of virus circulation or disease burden – let alone representative of the full array of pathogens, known and unknown, that could be associated with respiratory illness.
Flu Deaths: Cause or Effect?
Death is the ultimate measure of flu season severity (and disease severity in general). If the overall or age-group rate of flu-attributed deaths is higher in a season, it’s characterized as a “worse” flu season.
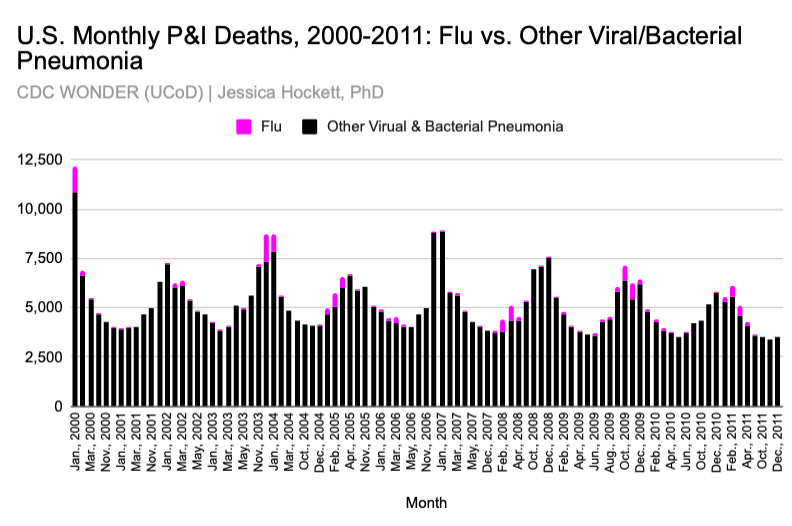
In recent decades, the CDC has combined deaths attributed to influenza per se with deaths attributed to pneumonia (regardless of causal agents) and called these “P & I” deaths. Like all deaths, these are associated with specific codes and coding guidance from the WHO International Classification of Diseases (ICD). The flu and pneumonia codes are located in the Diseases of the Respiratory System chapter. For now, I’ll refrain from explaining or debate the wisdom of the various codes. Suffice to say, there are different manifestations and causal or coincidental agents of pneumonia, one of which is influenza. Sometimes a virus or bacterium is identified for a pneumonia death; other times it is not.
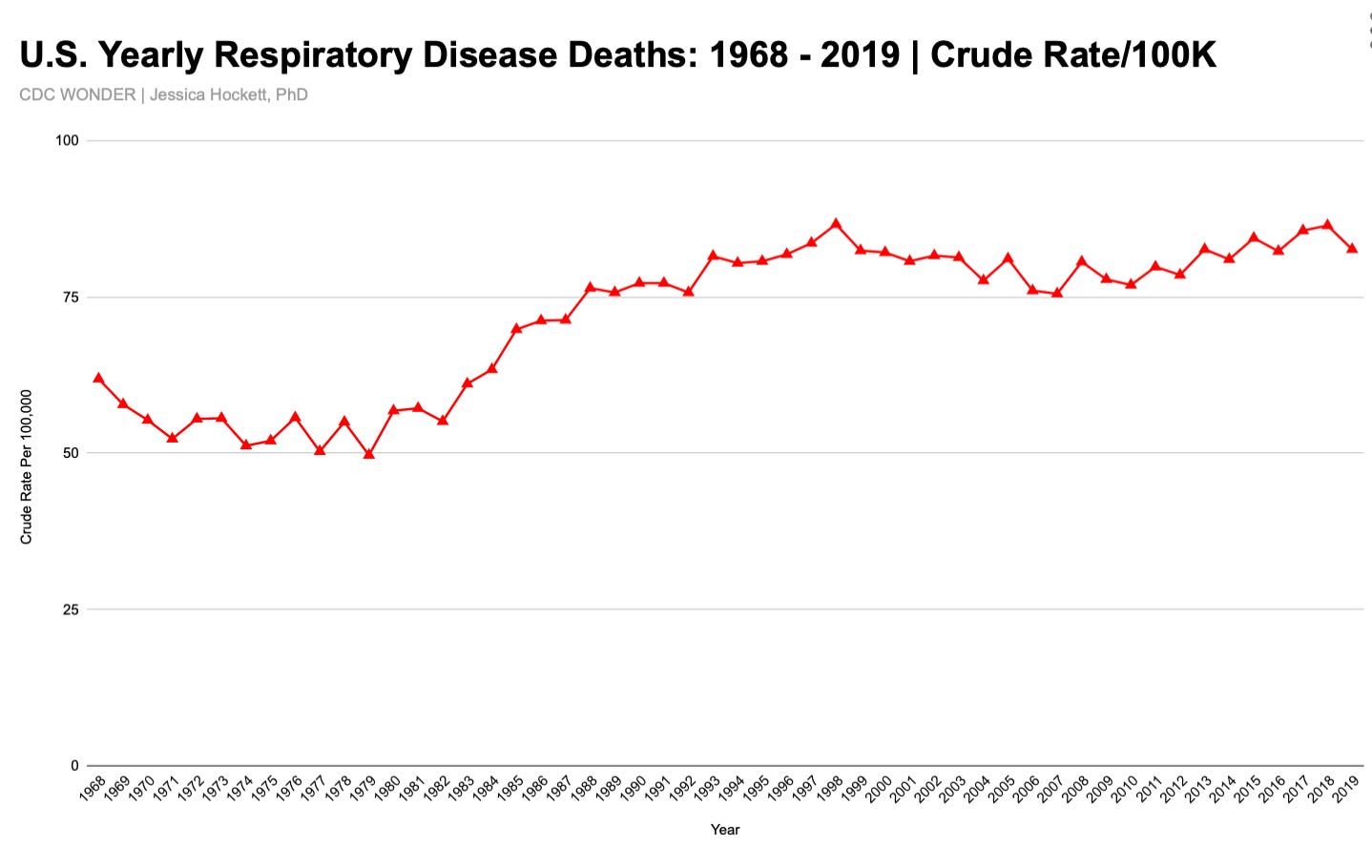
Federal data from 1968 - 2019 shows the crude rate of respiratory disease deaths (including P&I) in the U.S. rose in the early 1980s, peaked in 1998, and remained fairly steady thereafter (Figure 10).
Figure 10
Since 1999, the raw number and rate of P&I deaths has declined, though not by much (Figure 11). The same is true with P&I deaths Americans age 75 and older, who are more susceptible not only flu/pneumonia, but to death.
Figure 11
The government and other vested parties would like the public to believe this means that efforts to surveil, vaccinate, or treat flu are working. Yet cause of death attribution is more fungible than people think. Determining the manner and cause(s) of an individual death can be straightforward, but not always.
Former death certificate clerk Joy Fritz explains this well:
“Most of us assume mortality statistics are exempt from Mark Twain’s saw about statistics being lesser in value to lies and damn lies. But the nature of cause-of-death data capture belies the reliability of mortality statistics as structurally sound. Mortality statistics tabulated from death certificates should not steer public health recommendations or medical decisions. Using them as a metric for scientific research or public policy is about as prudent as building a skyscraper on a sandbox.”
This perhaps has been more obvious since 2020, with deaths blamed on Covid-19, but has really always been the case. Everything from social and medical trends, time constraints, bureaucratic requirements, financial or political incentives, and zeitgeist/ortgeist can impact what a death certificate ends up saying (or not saying).
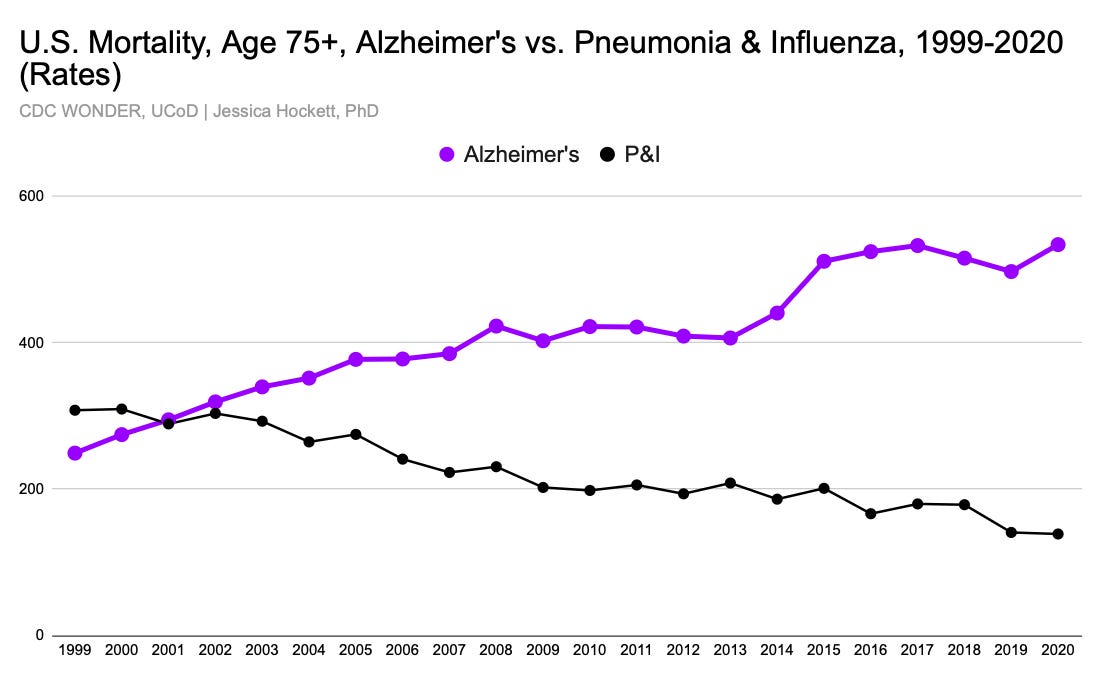
Trends in Alzheimer’s deaths, and their relationship with P&I deaths, are a good example. The rate of Alzheimer’s deaths among the oldest age groups has more than doubled since 1999. The Society of Actuaries observed that, early in the trend, Alzheimer’s stole deaths from death categories.14 This includes P&I deaths, which show an inverse relationship with Alzheimer’s, as an underlying cause.15 Since 2000, as the rate of one has gone up, the rate of the other has gone down (Figure 12) Whether this a coincidence, a shift in priorities, or something else, we can’t be sure. Incentivizes such as research funding and the need to show that shots or other treatments work can’t be ignored.
Figure 12
For all the fanfare, H1N1 failed to generate excess death, or even impact total P&I deaths (Figure 13) It’s hard to sustain panic (and profits) over a pathogen if people aren’t dying from it and your shot doesn’t deliver — or, worse, creates more harm than the disease.16
Figure 13
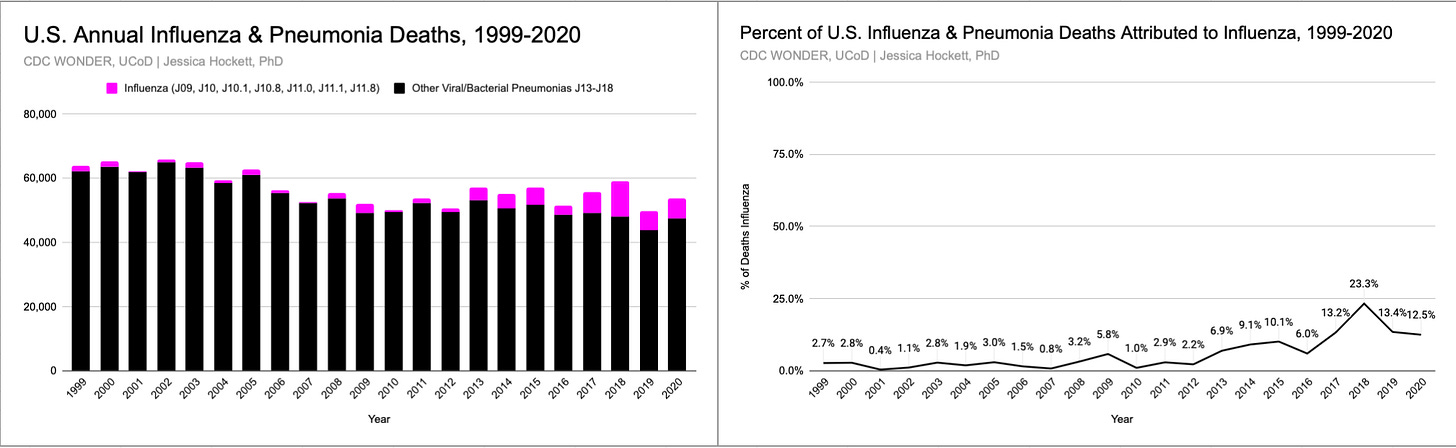
But, it may not have been a bust from another point of view. Note that the proportion of flu-attributed deaths in the P&I category has shifted markedly toward the influenza codes since 2013. This matches the overall increase in flu testing and flu positives in these years (Figure 14)
Figure 14
Still, the WHO/CDC Swine Flu Venture was successful in what it demonstrated about testing. Specifically, that testing could be leveraged to a) get the public’s attention, b) justify the pandemic preparedness industry, c) expand global disease surveillance programs, and d) pin more P&I deaths on influenza.
The Stage is Set
Readers will take away different things from this stage-setting; my bottom lines are these:
Flu surveillance data are a reflection of decisions and reactions – not just patterns of illness, symptom severity, or prevalence of causal pathogens.
The 2009 swine flu scare is a prime example of how, via media, government and health officials are able to direct or affect healthcare seeking behavior and capture results of that behavior through a new test for a new detection of a pathogen. And not just any pathogen, but one that ostensibly “needs” a shot or other profit-generating treatments.
Trends and patterns in cause-of-death attribution reflect myriad factors and forces. What a death certificate says isn’t a simple matter of medical science.
H1N1 seems to have ushered in an era of more aggressive flu testing that shifted the proportion of P&I deaths toward influenza codes.
I’m realizing that it’s relatively easy to create the appearance of an impending flu pandemic, especially when the public isn’t seeing all data in concert or in context.
The harder part is making more people die.
Some of the content in this post has been inspired by the work of my friend @professorakston, who also gave feedback on an earlier draft of this post. I recommend his April 25, 2020 video “SARS, H1N1, and Now Covid-19: Why We Keep Getting This Wrong.”
Other people who have written and/or produced media about the flu disappearance - including some with whom I disagree - are John Cullen, Martin Neil & Colleagues, Bill Rice, Jr., Jordan Schachtel, and Eugyppius.
UPDATE (7/8/2023): I posted a thread with some of this content in this post, but an H1N1 focus on Twitter here.
When I use the word “pandemic,” I am acknowledging the use of the term by health agencies and media. I am not validating any pandemic declarations, which I generally consider circumspect and unsubstantiated.
For recent examples, see Tim Sherman’s thread on a flu pandemic predictions and preparedness push in 2017 and 2018. Proceedings from a June 2004 workshop hosted by the Institute of Medicine's Forum on Microbial Threats, published by National Academies Press as “The Threat of Pandemic Influenza,” are also representative of the pandemic preparedness ethos and plans.
Hawaii is an exception, which sees year-round circulation, with less exaggerated peaks.
e.g., family practice, pediatricians, ER physicians, urgent care centers, public health clinics, university health centers
The CDC sets baseline and threshold values for these for declaring an epidemic. The overall trend of both the baseline and threshold values over the past 15 years is downward -- and was revised downward again in 2020.
I suspect Respiratory Virus Panel (RVP) testing has proliferated since 2012 - and are correlated/contribute to the specimens tested/testing positive for influenza - but I’ve yet to investigate fully.
The full guidelines updated in 2018 are from the Infectious Diseases Society of America.
With SARS-CoV-2, this didn’t happen. A delay in test availability and deployment made the public, healthcare providers, and those in public health misinterpret the rise in positivity for the disease spreading.
The same is true in state-level data (e.g., North Carolina).
A memo from the Illinois Department of Public Health indicates that a separate test was (and is?) needed to subtype H1N1.
“Stole“ is my term, not the Society of Actuaries’ term. They say, “Some of the early increases [in the Alzheimer’s death rate for age 85+] may have been due to the increased attribution of deaths to Alzheimer’s, away from other CODs.”
The efficacy of the many kinds of seasonal shots for influenza is beyond the scope of this post. However, some independent analysts have observed an association between the debut of the quadrivalent shot in 2014 and an increase in Alzheimer’s death rate. Moreover, flu shot efficacy among the elderly is not strong. "Residents of long-term care facilities and hospitalized patients are at high risk for complications of influenza, even if vaccinated, because influenza vaccine effectiveness may be low, particularly in elderly persons." (Uyeki, et al, 2018)




Jessica,
Astute and sobering analysis.
I was part of the leadership team for H1N1 in 2009-2011. Ran the clinical trials testing vax in pregnant women and also in AIDS patients, at NIAID under Fauci. Oct 2009 we distributed the vax and then "positive tests dropped dramatically over Thanksgiving". Of course, we attributed it to our 'great efforts'.
Seen much differently now, in retrospect. Sigh.
Laura Kragie MD. biomedworks.substack.com
"WHO/CDC Swine Flu Venture was successful in what it demonstrated about testing. Specifically, that testing could be leveraged to a) get the public’s attention, b) justify the pandemic preparedness industry, c) expand global disease surveillance programs, and d) pin more P&I deaths on influenza. " Describes my several years of experience as a sentinel provider, then as an objector to the H1N1 HCW mandate in NYC - threatened with termination in 2009 and ultimately terminated in 2016. Finally, as an active primary and urgent care physician in NYC during the panic-demic of 2020, i will attest that everything you have observed in your research for this article reflects very accurately what I experienced in my day to day practice.